For drugs administered in clinics and hospitals, Medicare reimburses doctors a flat 6 percent of the price of the drug. This has never really made much sense, since it doesn’t cost any more to attach a $1,000 vial to an IV line than a $100 vial. So now the Obama administration is proposing a five-year test of a new system that pays a flat fee plus a smaller percentage of the cost of the drug. Here’s what it looks like:
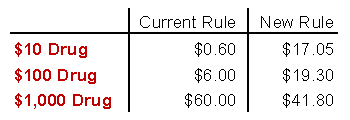
The current rule is an update of an older rule that was even stupider than reimbursing based on price. But it’s still pretty stupid. If two drugs are about the same, and you can make $6 from one and $60 from the other, then you might as well prescribe the more expensive one. That’s exactly the wrong incentive. Not everyone sees it this way, of course:
The test program is also likely to meet stiff opposition from the pharmaceutical industry and some providers—especially cancer centers where many high-price specialty drugs are used—because of the drop in reimbursement….Providers may also feel they are being pressured by the federal government into selecting cheaper drugs they don’t feel are as effective.
This makes no sense. No one is being pressured into selecting cheaper drugs. You just won’t get paid an artificial bonus for avoiding them in favor of more lucrative options that don’t work any better. If that’s your idea of “pressure,” I’d recommend you go into a less demanding field.
The new system, I assume, is designed to recognize that administering a drug is mostly—but not entirely—a flat cost operation. The reason the cost isn’t completely flat is that clinics and hospitals have to pay for the drugs up front and keep them in stock. There’s a carrying cost involved in that, which means that expensive drugs really do cost a little more to administer than cheaper ones.
But not that much more. The new system seems well worth a try.