Ebola has arrived in New York City. So should residents here be worried about a widespread outbreak? Almost certainly not: The disease is not airborne, and infected patients are only contagious once they show symptoms. Craig Spencer, the infected doctor in New York, has said he didn’t have symptoms Wednesday night when he rode the subway between Manhattan and Brooklyn and went bowling. Three people he came into contact with, who have not shown symptoms, have been placed in precautionary quarantine. And unlike West Africa, where health care is sparse and low-quality, the US is well equipped to handle cases of the virus; the hospital where Spencer is being treated has been preparing to treat Ebola patients. (Public heath officials in the city expected cases of Ebola to turn up sooner or later.)
But the prospect of a deadly disease outbreak in the Big Apple is still pretty scary, and the city hasn’t always dodged the pathogen bullet. Here are a few epidemics in New York that were far worse than Ebola is likely to be.
Yellow fever (1795-1803):
The city’s first health department was created in 1793 to block boats from Philadelphia, which at the time was in the grips of a yellow fever epidemic that left 5,000 dead. The tactic didn’t work: By 1795 cases began to appear in Manhattan, and by 1798 the disease had reached epidemic proportions there, with 800 deaths that year. Several thousand more died over the next few years. (The disease causes victims’ to vomit black bile and their skin to turn yellowish, and the fatality rate without treatment is as high as 50 percent.) This was no small blow for a city that at the time had only about 60,000 residents. As is the case today with Ebola in West Africa, misinformation was a big part of the problem: Doctors at the time had only just begun to speculate that the virus was carried by mosquitoes (other theorized sources included unsanitary conditions in slums and rotting coffee). Little effort was made to publicize the epidemic for fear of a mass exodus from the city, according to Baruch College. Today yellow fever is extremely rare in the United States but still kills 30,000 people every year, 90 percent of whom are in Africa.
Cholera (mid-1800s):

By the 1830s New York was a booming metropolis of 200,000, with swarms of newcomers arriving daily on boats from Europe. When word of a raging cholera epidemic in Europe reached the city’s Board of Health, it instituted quarantines on incoming ships and tried to clean up the filthy streets. But again the board was reluctant to make public announcements, this time to avoid disrupting trade, according to city records. One resident claimed the board was “more afraid of merchants than of lying.” By June 1832, the disease, which causes severe diarrhea and can kill within hours if untreated, arrived in New York via boats traveling down the Hudson River from Quebec. Within two months, 3,500 people were dead—mostly poor Irish immigrants and blacks living in the city’s slums. Outbreaks occurred again in 1849, with some 5,000 deaths, and in 1866, with 1,100 deaths.
Polio (1916):

New York City was the epicenter of an outbreak of polio in 1916 that began with a handful of cases reported to a clinic in Brooklyn. The disease, which advances from feverlike symptoms to paralysis and sometimes death, ultimately spread to 9,000 New Yorkers and caused 2,400 deaths. Across the Northeast, the infection toll climbed to 23,000 by the fall. The disease remained prevalent in the United States until the 1954 introduction of Jonas Salk’s polio vaccine. Polio is now extremely rare here. But worldwide, it still infects 200,000 people every year, particularly in Afghanistan, Nigeria, and Pakistan.
Influenza (1918):
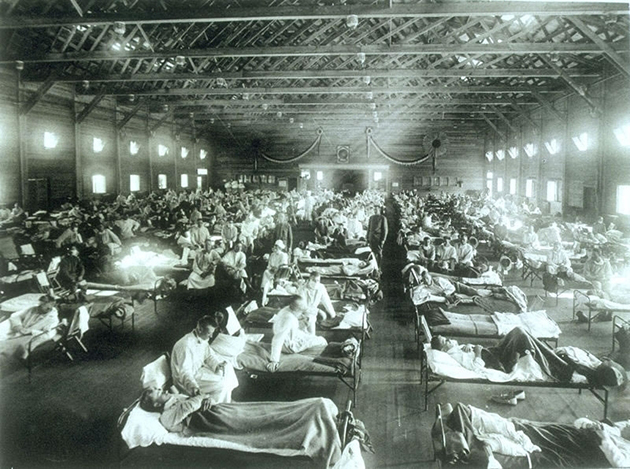
In August 1918, a Norwegian ship called the Bergensfjord pulled into New York Harbor carrying 21 people infected with a new and virulent strain of the flu. Over the next several weeks, dozens more arrived, mostly on ships from Europe, and sick passengers were quarantined in a hospital just blocks from the modern-day Bellevue, where Spencer is currently being treated. Those unfortunate sailors were just the first in what would become the deadliest disease outbreak in the city’s history to that date. Over 30,000 deaths were recorded by November—the actual number was likely much higher—including 12,300 during the first week of November alone. One health worker visited a family in lower Manhattan and found an infant dead in its crib and all seven other family members severely ill.
Other nearby cities fared even worse: The death rate in New York was 4.7 per 1,000 cases, compared to 6.5 in Boston and 7.3 in Philadelphia, according to the National Institutes of Health. That may not sound like a lot, given that the Ebola death rate is closer to 50 percent, but because influenza is so easily spread it can infect a much greater number of people. Globally, the 1918 flu killed between 50100 million people, the worst public health crisis in modern times. Today, the flu is still considered the greatest infectious disease risk for Americans, killing between 3,000 and 50,000 every year, according to the Centers for Disease Control and Prevention. In other words, it’s possible that more people could die from the flu this year in America than have died worldwide from Ebola during this outbreak. And yet only 1 in 3 Americans get a flu shot. Get a flu shot, people!
HIV/AIDS (1981-present):

The scourge of HIV/AIDS is the most familiar epidemic for modern New Yorkers, beginning with the June 1981 discovery of 41 cases of a rare cancer among gay men across the country. Throughout the 1980s, campaigns by the city encouraged New Yorkers to use protection during sex and not to share needles or use intravenous drugs. By 1987, according to city records, $400 million had been spent on AIDS services. But activists for AIDS rights groups like ACT UP accused city officials, led by Mayor Ed Koch, of dragging their feet and ignoring the true scale of the crisis. It took until the mid-’90s for anti-retroviral drugs to become widely available. Today, for people who have access to adequate health care, HIV is often manageable. But to date, more than 100,000 New Yorkers have been killed by AIDS-related maladies, according to state health statistics. Despite recent advances in medical treatment, infection rates are still high in New York, disproportionately affecting racial minorities and gay men.