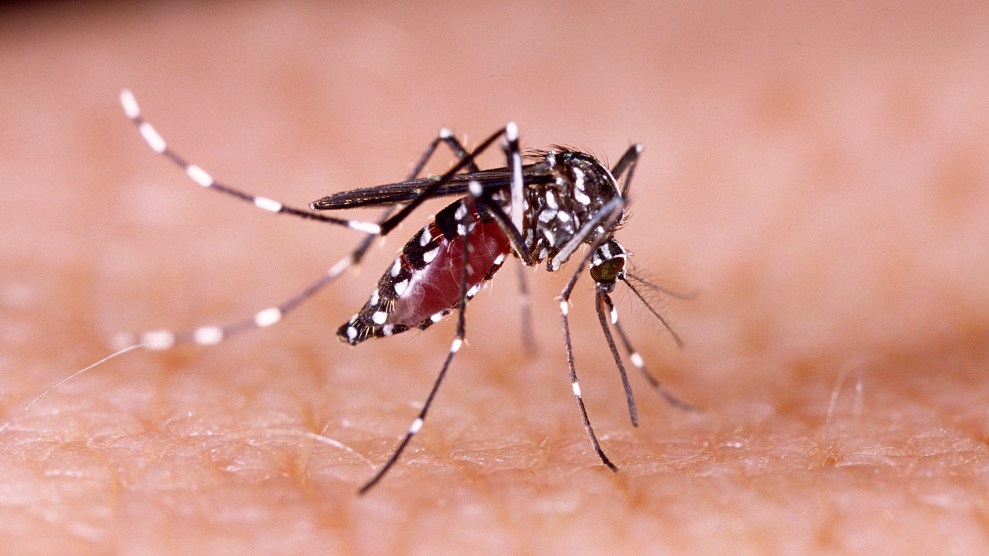
The Zika-transmitting Aedes aegypti mosquitoiStock/Tacio Philip
On Tuesday, with the Olympics fast approaching and the world freaking out over the runaway Zika virus, the Senate is expected to approve at least $1 billion to help keep the scourge in check. Several bills are up for consideration, and they all include a decent chunk of change for the development of a Zika vaccine, a task already well underway over at the National Institute of Allergy and Infectious Diseases. I figured it was a good time to check in with the institute’s longtime director—rock star scientist Dr. Anthony Fauci—to discuss how things are going, what we know (and don’t) about the epidemic, and whether we should just run like hell from the Olympics in Rio—where the Zika infection rate is estimated to be triple Brazil’s national average.
Mother Jones: I’ve read that a DNA vaccine for Zika could be ready for testing as early as September.
Anthony Fauci: Correct. But people get confused about this. It’s a phase I trial, just the first in a multiphase process of developing a vaccine. We took a DNA construct that we used to develop a West Nile vaccine a few years ago and we just substituted the Zika insert for the West Nile insert, so now it’s a Zika vaccine. We’re producing it in a pilot plant and doing all the preclinical studies you have to do before you go into a human, and we’re pretty certain we’ll get started with the trial in September. It usually takes three to four months and would typically involve around 80 volunteers. So let’s say we figure out that the vaccine is safe and that it induces the kind of immune response we would predict would be protective. If everything looks good, we’ll move into a larger (phase IIb) trial to determine if it’s effective.
MJ: And that would involve rolling it out in Zika-affected areas?
AF: Yes. Otherwise you’d never have enough infections to prove it’s effective. When you finish phase II is dependent on factors that are very difficult to predict. The two major factors are, one, how effective the vaccine is—because the more effective it is, the easier it is to prove it’s effective. The other factor is how many infections are going on in whatever country we’re testing it in: Brazil, Colombia, Puerto Rico, Venezuela—it likely will be multiple sites. If there is a lot of infection, we can probably determine within a year, by the beginning of 2018, if it’s effective enough. And then, depending on the urgency, you can get accelerated approval. Or, the FDA and other regulatory agencies may say you have to test it for another year or so.
MJ: If you need a lot of infections to determine whether a vaccine is effective, then how did you test the vaccine for West Nile, which has resulted in relatively few cases?
AF: We never tested its efficacy. We tested the West Nile vaccine the same way we’re going to do the phase I here. The problem is, we could not get any company to partner with us for advanced development because there was not the perception by any company that this was a vaccine that would be widely used. So we never brought it into phase IIb.
MJ: What are the pros and cons of a DNA vaccine versus, say, using an inactivated virus?
AF: It’s about the same. We have four or five candidates lined up. The first is the DNA. The one behind it is a whole inactivated [virus] particle vaccine. That won’t go into phase I until at least the end of 2016. Then we have a live chimeric inactivated vaccine that won’t go into phase I until the middle of 2017. But there’s no substantial difference. The DNA so far looks pretty good with regard to immunogenicity [strength of the immune response it elicits]. From a historical standpoint, whole attenuated [virus] vaccines tend to be more immunogenic. You’ve got to be careful with mice, you can’t be strictly extrapolating to humans, but in the studies we’ve done, just a few weeks ago, the DNA vaccine looked very immunogenic in a mouse, so it may be as immunogenic as the whole killed [virus].
MJ: How does a DNA vaccine work?
AF: You have a circular plasmid of DNA. You splice into it the gene of the Zika outer coating protein. You inject that plasmid into the muscle of an individual. It goes into the host cells and starts to produce the protein, which your antibodies attack. Interestingly—this is good luck—the vaccine doesn’t just produce soluble outer envelope proteins, it produces them in the form of a virus-like particle. So they look like a small virus, which makes them that much more immunogenic.
MJ: Some researchers worry that Zika is stimulating an autoimmune response in some adults that makes the body attack its own nerve cells, and that’s why we’re seeing these Guillain-Barré symptoms. If that’s what’s happening, is there a danger that a Zika vaccine could actually cause Guillain-Barré?
AF: In these small safety studies, if there is a complication like that, it’s probably so rare you wouldn’t pick it up. That’s why, when you do a larger study, you have to do double-blind, placebo-controlled trial. Because whenever you’re developing a vaccine that could have a deleterious effect, you want to make sure you’re not seeing worse effects in the vaccinated than in the unvaccinated. And when dealing with any vaccine, there’s always the danger—and we’ve seen this with flaviviruses [which include Zika and dengue], so you have to be careful—that if you have an inadequate antibody response, you can actually enhance the infection.
MJ: I’ve read that with dengue, people who get re-infected after a previous infection are at much higher risk for the extreme form of the illness.
AF: It’s called “antibody-mediated enhancement.” Let’s say you get infected with serotype 2 dengue and then you wind up getting infected with serotype 4. The antibody against serotype 2 is good enough to protect you against reinfection with serotype 2, but even though it cross reacts somewhat with serotype 4, it’s not good enough to protect you. And when it binds to the [serotype 4] virus as it enters your body, sometimes it enhances the ability of the virus to damage your tissue. That can be the scenario for developing the hemorrhagic dengue syndrome.
MJ: Are we worried that something like this could happen with Zika?
AF: Well, interestingly, the Zika that’s going around in Brazil is all one serotype. So that’s not so much of a concern.
MJ: The Senate is preparing to approve a good-sized sum for Zika vaccine development. How will that accelerate your efforts?
AF: It won’t accelerate it. It will allow it to happen. You can’t rush clinical trials. If we didn’t get the money, it would either be dramatically slowed down, or it wouldn’t happen.
MJ: At a recent Zika summit, you said, “I have this ominous feeling we have yet to see the worst of it.” What were you thinking about when you said that?
AF: It was at a time when every time we would learn something new, it would not be good news. First it was. “Is it really causally associated with the congenital abnormalities of microcephaly?” Well, we don’t know—then all of a sudden we definitely know: The first cohort study showed a 29 percent incidence, which is really very high. Then we find out when we study the virus in vitro—either in a test tube using these organoids, or in a mouse model—we find out the virus is ferociously neurotropic; it really destroys neurological tissue very aggressively. [Scientists asked], “Well, is it something special with Brazil? Is it a co-factor with dengue?” Uh-uh. It can do it by itself. And then you find out it’s sexually transmitted. Now if you ever wanted to compound and confound the spread of an outbreak that already is amazingly strange—the first mosquito-borne virus that results in a congenital abnormality—now you find out it’s sexually transmitted! And then you find out it’s also associated with Guillain-Barré. I was saying, “My goodness. Every time you wake up, there’s something else that’s bad about it.”
MJ: Okay, along those lines, given that Zika attacks developing nerve cells, wouldn’t we expect it to go after the brains of adolescents, who are having all this explosive brain growth?
AF: Thus far, there’s no red flag that comes jumping out at us with young kids and adolescents. However, the only way you really know is to do a long-range, multi-year cohort study. You follow the children and find out if those who were infected young end up with mental abnormalities. Part of our cohort study is going to look at that. I don’t think we’re going to see it, but you have to look.
MJ: Roughly 80 percent of people infected with Zika never get sick. Does a pregnant woman need to show symptoms for her baby to be affected?
AF: We don’t know. So we’re doing a “Zika in infants and pregnancy” program—called a ZIP—to ask just that question. Do only symptomatic women have a problem with their fetuses? What’s the level of virus in an asymptomatic woman versus a symptomatic one? There are a lot of questions we’re going to ask. You just asked one of the important ones.
MJ: How do you even find asymptomatic people?
AF: You have to do a screening study of thousands of people in the community.
MJ: If a person is asymptomatic, can they spread Zika through sex?
AF: You’re asking all the right questions. It’s almost as if you looked at our protocols, because those are the questions we’re asking. So far, the only sexual transmissions that we know of are people who transmitted it when they were symptomatic or very, very soon after. In fact, the ones that are well documented had a rash when they transmitted it. But that’s maybe just the tip of the iceberg.
MJ: There’s been some debate over whether the Olympics should be moved or delayed. What’s your take?
AF: I don’t think so. You have to be careful and know what the risks are. You’re pregnant, might be pregnant, planning on being pregnant: Stay away from areas where there’s active Zika transmission. That’s the most important thing. If you’re an athlete who has no intention of being pregnant, you go down there, and apart from the Guillain-Barré—we don’t know how great the risk is yet—Zika is a relatively mild disease: fever, aches, pains, rash, conjunctivitis, and done. And that’s if you even show symptoms. But it’s really important to look at the guidelines: A) Pregnant? Stay away. B) If you’re a man, and you come back home to a pregnant wife, don’t have sex—or consistently use condoms for the duration of the pregnancy. If you don’t have a pregnant wife or girlfriend and really want to be safe, you use a condom for eight weeks upon returning. If people do that, there’s no reason not to go to the Olympics.
MJ: So far, we’ve had zero mosquito-borne Zika transmission in the United States, probably for the same reasons we haven’t seen much dengue here. Do you think we’re going to start seeing mosquito-borne transmission here?
AF: Yesterday was my sixth congressional hearing on this, not to mention many individual briefings, and I’ve been very consistent. We’ve had now 500 or so travel-related cases. We’ve had no local transmission. It is likely that we will have restricted local transmission—small local outbreaks? My call would be that we will. Because we’ve had dengue and chikungunya, which are in the same regions of South and Central America and the Caribbean, and are transmitted by exactly the same mosquito. Historically we’ve had small local outbreaks of dengue in Florida and Texas, and a small local outbreak of chikungunya in Florida, which makes me conclude that sooner or later, we have going to have small local outbreaks of Zika—whether that’s five cases or 30—likely along the Gulf Coast.
Having said that, the dengue and chikungunya outbreaks were well controlled by aggressive mosquito control and attention to using insect repellent, staying indoors with air conditioning, making sure you have screens in your house, and eliminating standing water in those areas. That successfully prevented dengue and chikungunya from becoming sustained and disseminated. So, I never say never, but I do not think we’re going to have a widespread Zika outbreak in this country.