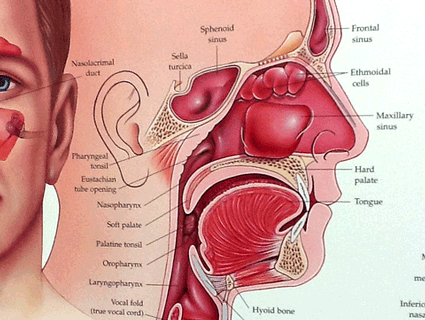
<a href="http://www.flickr.com/photos/44124483743@N01/6558021051/">brownpau</a>/Flickr
Sinus infections are nasty beasts. They leave you exhausted, drowning in green snot, seeing double from face pain, and ready to beg your doctor for antibiotics. Roughly 20 percent of all adult antibiotic prescriptions in the United States, it turns out, are written to treat sinusitis. In fact, I got one of those prescriptions just a few weeks ago, even though antibiotics are almost entirely useless for the condition, and may be causing more harm than good.
Antibiotics only kill bacteria, but a whopping 90 percent of sinus infections are caused by viruses, according to the Infectious Diseases Society of America. What’s more, new research over the past year has proven definitively that antibiotics won’t change the course of most sinus infections.
The rampant misuse of antibiotics to treat conditions they can’t possibly cure is one major reason for the alarming rise in the number of “superbug” outbreaks—infections by deadly bacteria that have evolved the ability to survive most antibiotics. (The other reason has to do with overuse of antibiotics by factory farms.) The more antibiotics you take, the more likely that you’ll develop a drug-resistant infection. That’s because, while the drugs kill most of the bacteria, the most naturally resistant ones are most likely to survive—and multiply.
The Centers for Disease Control and Prevention (CDC) has spent a decade trying to convince doctors to stop dispensing antibiotics for viral conditions in order to preserve the effectiveness of these crucial lifesaving drugs. Meanwhile, a host of medical specialty groups have launched a new “Choosing Wisely” campaign designed to educate patients about unnecessary treatments. The program specifically emphasizes avoiding antibiotics for sinusitis.
The CDC estimates that Americans and their insurers shell out $1 billion a year for worthless antibiotics prescriptions for upper-respiratory afflictions. But the collateral damage is more worrisome than the money: In the past several months, hospital have seen outbreaks of bacteria that are resistant to every antibiotic on the market and have killed about half of the people they infect. “Antibiotics are losing their effectiveness at a rate that is both alarming and irreversible—similar to global warming,” England’s chief medical officer warned last year as the European Union recognized that 25,000 Europeans were dying annually from drug-resistant bacteria.
The public-health campaigns to curb antibiotic use are not working especially well, as I discovered last month during a nasty bout with sinusitis. As someone with asthma, allergies, and a deviated septum (all known risk factors), I get sinus infections a lot, so while I waited around for my condition to improve, I read up on the latest treatment research. All of it said in no uncertain terms that antibiotics do not help, and practically screamed: “Don’t take them!”
After being sick for several days, I finally ventured out to see a doctor, even though I suspected there was nothing he could do. That was probably a mistake, as seeing a doctor for a generic upper-respiratory ailment like a sinus infection or bronchitis almost guarantees that you’ll end up violating the CDC’s advice.
Despite all the exhortations about antibiotic overuse, the ear, nose, and throat specialist I saw not only wanted to give me an antibiotic, he pressed me to take a powerful, broad-spectrum one called Levaquin, one of the few drugs effective against certain really deadly bacteria—like anthrax. For obvious reasons, the CDC strenuously warns against using this kind of drug indiscriminately.
Not only is Levaquin major overkill for a sinus infection, it has potential side-effects (psychosis, seizures, and liver and nerve damage, to name a few) that are far more horrible and serious than green snot. What’s more, the overuse of Levaquin is suspected as a culprit in the rise of the drug-resistant staph infection known as MRSA. It is quickly becoming impotent against things that people really need it for, like hospital-acquired pneumonia.
When I asked the doctor about all of this, he conceded that antibiotics weren’t called for in most sinus cases. Yet he urged Levaquin anyway, as I’d been sick for more than a week. I asked if he could “swab” me to make sure that I really had a bacterial infection before taking the drugs. He said by the time the culture results came back I’d be better regardless—which seemed like another argument against antibiotics. (The lack of a quick test for bacterial sinusitis is one of the major obstacles to reducing antibiotic overuse, because it forces doctors to play the guessing game.)
In the end, I left with a prescription for Augmentin, an antibiotic that the CDC recommends as the first-line defense against a bacterial sinus infection. I never filled it. One week later, the green snot was gone. But I’d missed six days of work in two weeks, and that’s when I realized why the CDC campaign will likely fail. I’m lucky enough to have paid sick leave, a sympathetic employer, and a union to help ensure that I can use my sick leave without losing my job. Most Americans don’t have this luxury. They’ll go to work even when they feel miserable, and beg their doctors to fix them—fast.
“We do have somewhat an unsympathetic work culture, and I do agree that that leads to this desire, this desperate seeking of some sort of quick fix,” says Dr. Lauri Hicks, the medical director of the CDC’s “Get Smart” program to curb antibiotic overuse. Hicks adds that half of all antibiotics in the United States are prescribed (in vain) to treat viral illnesses. “Unfortunately, with most of these illnesses, there is no quick fix.”
Doctors, the front line in this fight, haven’t responded well to the calls to rein in antibiotic prescriptions. Dr. David Lang, an allergist at the Cleveland Clinic’s Respiratory Institute, worked on the “Choosing Wisely” recommendations. He concedes, however, that he has trouble following his own advice. It’s difficult for doctors to admit to patients that there’s not much they can do, Lang laments. “With regards to sinusitis, it can be uncomfortable. There’s no question that when people come in to see me they’re not coming in at a high point,” he says. “Treating such patients can be a challenge because it takes a lot of my time to educate someone and to persuade them to understand that this illness is going to resolve in all likelihood without the need for an antibiotic.”
Lang adds that he sometimes will write an antibiotic prescription for sinusitis but tells the patient to wait a few days and only fill it if they don’t feel better—a strategy employed by doctors in parts of Europe. (The British national health service goes so far as to tell people with sinus infections not to go to the doctor at all unless they’ve been sick for at least a week and are getting worse. It also warns that these infections take at least two weeks to clear up, something American doctors seem reluctant to do.)
The CDC is encouraging doctors to resort to some old-fashioned tricks of the trade—an update of “take two aspirin and call me in the morning.” Along with urging treatment for the symptoms of sinusitis (things like pain relievers and decongestants), the agency created a prescription pad that allows doctors to officially order their patients to go home, eat chicken soup, and rest for a few days. “It really does help patients to have a written note or instructions, even if it’s basic,” says the CDC’s Lauri Hicks.
The problem is that not everyone has the option of going home to bed. Nearly 40 percent of all workers—and almost 80 percent of the lowest-wage ones—have no paid sick leave whatsoever. America is one of the only industrialized countries in the world that haven’t mandated it. (See map below.) This is one reason that American workers only take, on average, about 5 days off a year due to illness, compared with more than 16 in Germany, and 22 in Sweden.
![]()
Map source: McGill Institute for Health and Social Policy
Earlier this month, members of Congress reintroduced the Healthy Families Act, a bill that would require employers with more than 15 employees to let workers accrue 56 hours of paid sick leave annually, and bar companies from retaliating against people who have the gall to use it. (The bill also would allow people to stay home and care for a sick kid or other family member.)
The bill, first introduced nearly a decade ago, has long been touted as a desperately needed weapon against a potential influenza pandemic, when keeping the infected at home would be critical to saving lives. Research shows that it also could greatly reduce the spread of gastrointestinal illnesses, because workers without paid sick leave are concentrated in service jobs like restaurants and day care, where they are in the position to spread their germs far and wide.
The business community, naturally, hates the bill and has blocked its passage, just as it has fought state and local initiatives that would mandate sick pay. But those efforts are monumentally short sighted. Letting people stay home when they’re sick will, with luck, help us maintain our defenses so that when really scary things like the bubonic plague come along, we can send the drugs to work.

















