 This should be old news, but since a lot of people still don’t get this it’s nice to see it getting front page treatment from the Washington Post:
This should be old news, but since a lot of people still don’t get this it’s nice to see it getting front page treatment from the Washington Post:
The federal government will bear virtually the entire cost of expanding Medicaid under the new health-care law, according to a comprehensive new study by the Kaiser Family Foundation that directly rebuts the loud protests of governors warning about its impact on their strapped state budgets….Governors of many of those states have predicted fiscal calamity for their budgets, and some have cited the Medicaid expansion in the suits they have filed against the new law, saying it violates their states’ rights.
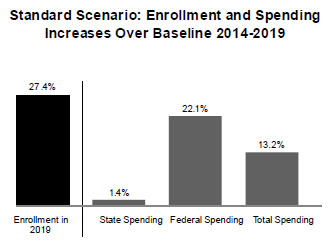
But the Kaiser study released Wednesday predicts that the increase in state spending will be relatively small when weighed against the broad expansion of health coverage for their residents and the huge influx of federal dollars to cover most of the cost.
Even the small increase in Medicaid costs may be canceled out by the savings states will enjoy from no longer having to subsidize the uncompensated care of uninsured people who will be on Medicaid, study co-author John Holahan said. “It’s absurd,” Holahan, an Urban Institute researcher, said of the states’ doom and gloom predictions. “They come out ahead. It’s just crazy.”
Bottom line: the federal government is paying more than 95% of the cost of the Medicaid expansion that’s included in the healthcare reform bill. In some states the federal share is even higher. Total state spending on Medicaid will go up only 1.4%, a grand total of about $4 billion per year to cover more than 11 million people. What’s more, it might be even better than that: as Holahan says, states might find that in the end they come out in the black on overall healthcare costs since their spending on care for the uninsured will go down. Keep this in mind the next time your state’s governor starts wailing about healthcare reform and how it’s going to bankrupt your state. It won’t. The full report is here.