There are plenty of reasons why the Obamacare repeal bill that House Republicans passed Thursday afternoon is so controversial. It slashes funding for Medicaid, threatens to raise health insurance premiums for older Americans, and allows states to roll back protections for people with preexisting medical conditions.
But there’s another, less publicized, way in which the GOP’s American Health Care Act could disrupt health care throughout the country. In the midst of the most devastating drug epidemic in US history, the legislation could disrupt addiction coverage for millions of Americans. And thanks to a provision added to the bill last week, insurance companies in some states might no longer include mental health and substance abuse coverage in their health plans.
Because of the speed with which Republicans rushed the bill through the House, the Congressional Budget Office hasn’t yet had time to estimate the number of Americans who would lose their health insurance or how premiums would be affected. But according to a CBO report from March, an earlier version of legislation would have resulted in 24 million fewer people having coverage than under Obamacare. The current legislation will likely result in a similar number of uninsured Americans, says Richard Frank, a professor of health economics at Harvard University. Frank and his colleague, Sherry Glied of New York University, estimate that if Obamacare is repealed, 3 million Americans with addiction disorders would lose some or all of their coverage.
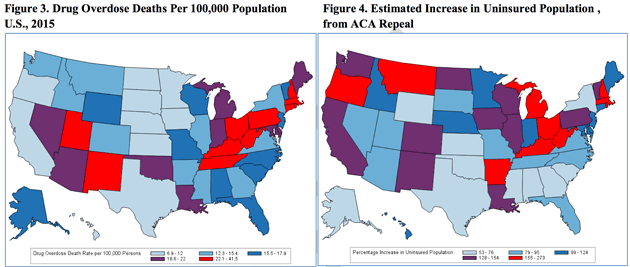
Many of the states that voted Trump into office are among the hardest hit by the opioid epidemic—and are the most dependent on Obamacare for substance abuse treatment. The maps below, produced by the US Department of Health and Human Services in the last days of the Obama administration, show this overlap: Red states on the left have the highest overdose rates per capita; red states on the right have the highest rate of residents who would lose coverage if Obamacare is repealed.
Obamacare was particularly important for those seeking addiction treatment, according to Keith Humphreys, a Stanford University psychiatry professor who advised the Obama administration on drug policy. “It was designed to be very broad, but at the same time we knew that if there was anything that this would help a lot for, it’s addiction,” he told me in February.
That’s largely because of two big changes that Obamacare made to insurance markets—changes that the GOP legislation would roll back or undo completely.
First, Obamacare required insurance companies to cover certain “essential benefits,” including substance abuse and mental health treatment. In order to sell insurance in the individual marketplaces, companies would have to cover addiction treatment, as well as other care such as contraception, emergency services, and pediatric services. (Here‘s the full list of essential benefits.) This was a significant change. In 2011, before Obamacare went into effect, “somewhere close to 40 percent of individual and small group market plans didn’t offer substance abuse and mental health coverage,” says Frank. “And when they did, it was quite limited.”
The bill passed by the House would allow states to opt out of the essential benefits requirements, which means that insurers might once again refuse to cover treatment for mental health and addiction.
The second big Obamacare change for substance abuse treatment was the expansion of Medicaid coverage to millions of additional poor Americans. As I wrote earlier this year:
Under the Affordable Care Act, those who earn up to 138 percent of the federal poverty level are eligible for this government-funded insurance program. In 2012, the Supreme Court ruled that states could choose whether or not they wanted to participate in the program, and 31 states have done so—resulting in health coverage for an additional 11 million Americans through Medicaid expansion. Of those, an estimated 1.3 million used their newly acquired insurance for substance abuse or mental health services, according to an analysis by researchers Richard Frank of Harvard Medical School and Sherry Glied of New York University. In states that expanded Medicaid, 20 percent of hospital admissions for substance abuse and mental health disorders were uninsured in 2013, before the bulk of the expansion provisions kicked in. By the middle of 2015, the uninsured rate had fallen to five percent.
The Republicans’ health care plan would freeze Medicaid expansion, cutting off funds for states adding new enrollees starting in 2020. Those already enrolled in Medicaid expansion plans by 2020 would continue to receive the benefits, but they would be at constant risk of losing that insurance. Anyone who has a gap in insurance coverage of more a month—say because they miss a deadline or their income temporarily changes—would lose eligibility. (A lack of private health insurance would be penalized too: Going more than 63 days without coverage would increase premiums by 30 percent for a year.) These provisions have a lot of public health advocates worried. It’s not uncommon for people, particularly those with serious mental health and addiction problems, to drift in and out of insurance coverage.
Without Obamacare, said Humphreys, “We’re back where we were before: bad access, low quality of care, and a lot of patients being turned away.”