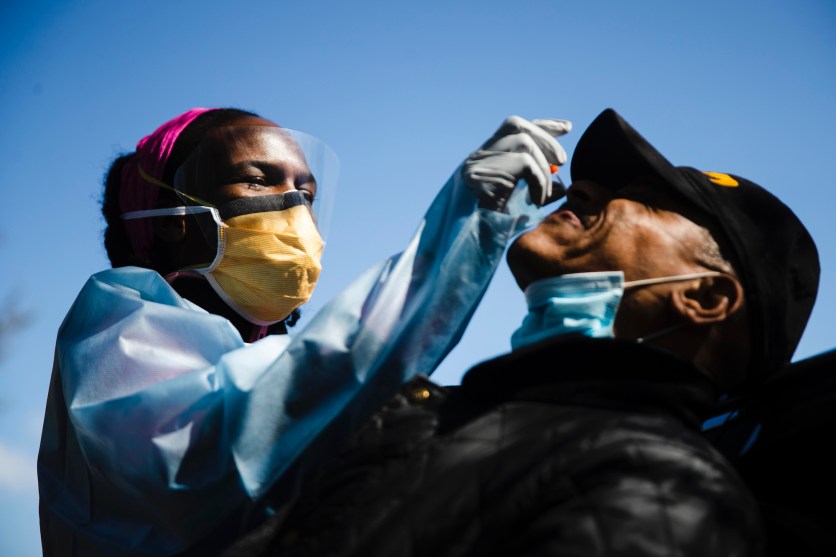
Dr. Ala Stanford administers a COVID-19 swab test on Wade Jeffries in the parking lot of Pinn Memorial Baptist Church in Philadelphia, Wednesday, April 22, 2020. Stanford and other doctors formed the Black Doctors COVID-19 Consortium to offer testing and help address heath disparities in the African American community. (AP Photo/Matt Rourke)
This piece was originally published in Yale Environment 360 and appears here as part of our Climate Desk Partnership.
While cities and towns across the United States are wrestling with the devastating impacts of the coronavirus pandemic, none have been hit harder than low-income and minority communities. Places like Detroit, Chicago, and St. James Parish in Louisiana, plagued by decades of economic inequality and pollution in impoverished neighborhoods, have experienced some of the country’s highest mortality rates from the virus. Recent studies have shown a link between high levels of pollution and an increased risk of death from COVID-19.
Sacoby Wilson, an environmental health scientist at the University of Maryland, believes the coronavirus has cast a spotlight on largely unnoticed segments of society, from low-income people in polluted neighborhoods, to residents of nursing homes and prisons, to workers in the nation’s meatpacking plants “One thing that COVID-19 has done, it has made a lot of populations we made invisible, visible,” Wilson says in an interview with Yale Environment 360.
In the interview, Wilson, who has spent more than two decades focusing on environmental justice issues, talks about why it is important to examine the pandemic through the lens of environmental justice and explains how the Trump administration’s moves to suspend enforcement of environmental regulations during the current crisis reflect a broader disdain for low-income communities. “I think it is a slap in the face to many communities affected by environmental injustice because it says, ‘We do not care about you,'” he says.
This interview has been edited for length and clarity.
The COVID-19 crisis has made it very apparent that low-income communities and communities of color are being disproportionately affected by the virus and the crisis. What are the major reasons for the disparity we’re seeing right now?
In this country, we have structural inequalities that are a major driver of why we see these different social and environmental conditions in communities of color. You see these different patterns of land uses, whether it be transportation networks, large highways where you have a lot of traffic, or industrial activity. There’s a recent Harvard study that shows that with long-term exposure to PM2.5 [fine particulate air pollution], there’s an association with higher mortality rates for individuals who had a COVID-19 infection. We have a pattern in this country, where communities of color and low-income communities host more of these [heavily polluting] land uses. I think that has played a major role in why we see the disparate impacts of COVID-19 as it relates to morbidity and mortality rates.
You mentioned the study last month from Harvard showing that higher levels of air pollution were linked to an 8-percent rise in the COVID-19 death rate. What are the ecological and socio-economic reasons behind this?
Environmental regulations in this country, they’re not color blind. If the laws and regulations were enforced fairly across all racial ethnic groups, we wouldn’t have environmental injustice. Why do we have communities with more sources of pollution? Well, that could be because those communities don’t have a strong political voice. In many cases, in white, higher-income communities, you have more political power because of your economic power. So this NIMBY-ism, ‘Not In My Backyard,’ can stop an incinerator, stop a landfill, stop a highway from being built in those neighborhoods. Whereas, a lower-wealth community of color, because they don’t have the economic capital which drives their political capital, they don’t have the capacity to prevent the siting of those types of things in their community.
There’s a link between race and class in this country. In many communities of color, industrial developments are seen as economic opportunities. So, you are bringing in these industries that may provide jobs, but what you get instead is the pollution that is produced. And so, there’s a cost/benefit analysis that doesn’t really look at the true costs of, say, bringing a power plant into a community. The true cost-accounting of bringing a highway into a community, or a landfill, a refinery, a factory, a chemical facility, or a paper mill. What happens is you have these environmental externalities, the pollution impacts, from the facility. And then, you have the health impacts. We have a lot of black and brown communities, a lot of Native American communities, a lot of immigrant communities that are basically sacrifice zones because they are the dumping grounds for these pollution-intensive facilities.
But what’s more egregious is we’re not really using advanced science to understand the true exposure profiles of those local populations. What I mean by that is, you have a facility that may be releasing multiple chemicals into the air, water, and soil. Now, our national air quality standards really only have six [major] air pollution criteria. But we emit way more chemicals from these facilities than are included under that criteria. So, we may be tracking fine particulate matter or ozone or nitrogen dioxide, but we’re not tracking the release and health impacts of the numerous chemicals that may be released in that petrochemical operation or that incinerator. So, when you add on a second facility, then a third, fourth, or fifth in a community, we have not done a good job of understanding the aggregate exposures. So, PM2.5 is a pollutant that, it was shown in the Harvard study, could increase mortality rates with COVID-19. Now PM2.5 itself causes asthma, heart disease, stroke. It elevates blood pressure. It increases infant mortality rates. It can cause birth defects. It can cause low-birth-weight births. It also can cause diabetes, cancer, premature mortality. That’s PM2.5 by itself. What if you add ultra-fine particles? What if you add black carbon, which is a byproduct of diesel exhaust?
Part of the problem with the Harvard study is that it only looked at PM2.5. It doesn’t capture everything that people are exposed to in these communities. So, it’s probably an underestimation of the true risk of COVID-19 mortality associated with air pollution because we are not capturing all the pollutants that these communities are being exposed to.
Part of the reason why folks have a higher risk of mortality, when you have a COVID-19 infection and if you have asthma, you have reduced lung capacity. Your lungs are not as healthy as someone who has not been exposed to these pollutants. One reason African Americans or Latinos are dying from COVID-19 at rates higher than the other populations is because of underlying health conditions like diabetes, heart disease, and asthma. But your diet and behavior is driven by your context. If you only have fast food in your neighborhood, and you don’t have access to a grocery store, what are you going to eat? If you don’t have access to healthcare in your neighborhood and you don’t have insurance, what are you going to do? And, when you do have access, it may be poor-quality access. Context matters. Place matters. I want to emphasize that point.
Are there any specific communities or regions in this country that exemplify this issue? Areas that have major industrial centers that have shown higher COVID-19 mortality rates?
One hotspot you can look at is Detroit. Detroit is an international corridor. You have ports. You have warehouses. You have rail. You have a lot of truck traffic coming into Detroit from Canada. So you have a lot of particulate pollution, and a lot of adverse health effects like asthma, heart disease, stroke, and cancer. You also have a lot of industrial operations—power plants, refineries, like the Marathon facility. So you have parts of Detroit that are highly industrialized, that they have made sacrifice zones. You see the intersection of race, class, place, and invisibility. The city has experienced one of the nation’s highest mortality rates from COVID-19.
One thing that COVID-19 has done, it has made a lot of populations we made invisible, visible. Nursing home populations. The meatpacking industry. Prisons. Communities impacted by environmental injustice. These are communities that we’ve thrown away. We’ve made them invisible, but COVID-19 has made them visible.
The Trump administration announced in March that it was suspending enforcement of environment regulations during this crisis. I’m wondering, in your opinion, why that decision is particularly dangerous from an environmental justice standpoint.
That decision is a slap in the face to many communities affected by environmental injustice because it says, “We do not care about you.” Whether it be a national disaster, a chemical or technological disaster, or a biological disaster like COVID-19, they are always the most vulnerable communities in many cases. And so, when you make a pronouncement that the model rules and regulations won’t be enforced in a pandemic, it basically says to corporations, industries in those communities, “Hey this is the wild, wild West. Do what you will. We’re not going to regulate you. We’re not going to have any oversight.”
The administration has continued its environmental legislative rollbacks during this crisis, weakening the mercury rule from power plant emissions, lowering fuel economy standards. Which of those rollbacks would be the most harmful for low-income and minority communities?
You have Clean Air Act rollbacks. You have Clean Power Plan rollbacks. You have a rollback of a law about hurricane-related flooding. You have the rollback of the automobile [mileage] standards. It’s the totality of these rollbacks that’s really problematic for communities already impacted by environmental injustice. Part of the problem, in my opinion, is laws and regulations were not enforced equally before this pandemic and before this administration. Because environmental justice wasn’t taken as seriously as it should have been under the Obama administration—even though Obama did much better than the Bush administration—we haven’t made as much progress as should have been made post-Katrina. Previous EPA [Environmental Protection Agency] administrations and the Office for Civil Rights didn’t do the best job in advancing environmental justice and forcing various rules and regulations to protect communities that have environmental justice issues. And so, it created fertile grounds for the issues, the concerns, the challenges that these communities deal with to be dismissed during this pandemic.
As we edge closer to summer and the coronavirus crisis continues, what impacts will hotter temperatures have on these communities and their ability to cope with the virus?
That’s a really important point. This year marks the 25th anniversary of the Chicago heat wave. You have a lot of communities pre-COVID-19 who were at risk from heat-related morbidity/mortality. They may have poor-quality housing, and housing with limited air conditioning, and limited access to other resources that allow people to stay cool during summer weather.
So, for folks who are in neighborhoods and communities that have had high case rates of COVID-19, communities that may have, again, limited access to healthcare infrastructure, communities that may be dealing with a lot of air pollution issues, you’re going to see, I think, compounded risks and increased mortality risks related to COVID-19 and also related to heat. They’ll have to make a choice. Do I leave to go to a cooling unit if I don’t have AC and then be exposed to the virus in those settings? Part of the problem is, when you go to a cooling station that’s indoors, it’s all a connected HVAC system so it’s going to recirculate the air, unless you have really good systems that bring in fresh air from outside to remove the contaminated air. Basically, you’re creating this exposure bubble, a toxic bubble, where people who are leaving their home to get cooler may end up being exposed to the virus because they’re going to an environment where people may be symptomatic or asymptomatic.
Low-income communities and communities of color have long borne the brunt of the impacts of national disasters, such as Hurricanes Katrina and Maria. Have policymakers learned anything from these events and, if not, what lessons should they be learning now?
Hopefully they’re learning that to make communities more prepared for these disasters you have to invest in those communities and not just invest in jobs. I mean invest in transformative change where we make those communities healthier, more viable, ecosystems. Make changes in communities so they’re not hosting these polluting land uses that can decrease their lung function or their cardiopulmonary/cardiovascular functions, so they can be more resilient to a biological agent like COVID-19. We need to invest in public health preparedness as it pertains to disasters, whether it be the next Maria, Katrina, Sandy, Florence, or Harvey. Whether it be the next 10-day, 20-day heatwave in Chicago or in Maryland or in some location where you have elderly folks or children who don’t have access to air conditioning. Whether it be the flu outbreaks, or dealing with the next COVID-19. There are lessons we can learn from this about how we do better preparedness.
If we’re going to have a better response to biological disasters or the next climate or technological disaster, we have to understand how racism plays a major role in our policies and also how racism and these structural inequalities drive the Haves and Have-Nots. The Haves will get quick access to testing kits. The Haves can follow a stay-at-home order and be fine, like someone like me. I’m a professor. The Haves who have access to natural spaces and good access to air conditioning and energy efficient homes, good access to healthcare.
COVID-19 has shown that we have a lot of Haves in this country, but we have a lot more Have-Nots. Our policies have disproportionally benefited the Haves while disproportionately impacting the Have-Nots. To address the disparities in COVID-19, we have to address our structural inequalities in this country. The first place to start is race and racism.















