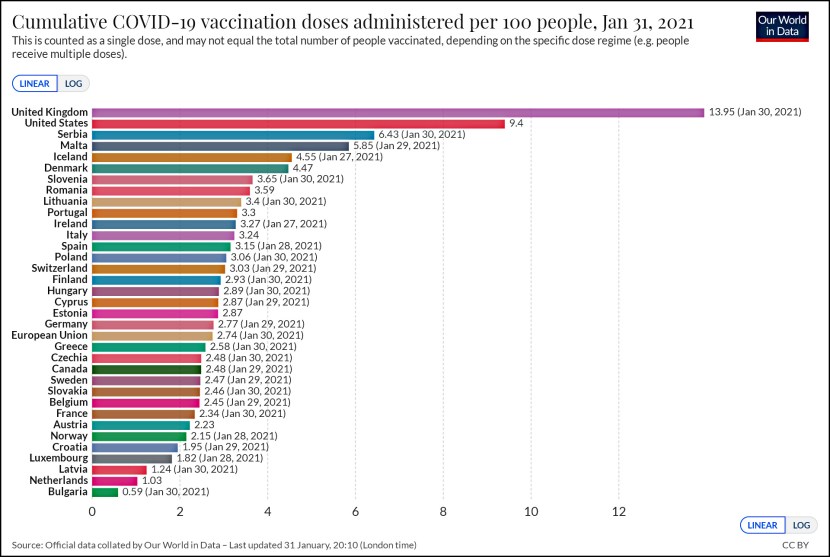
Via Bill Gardner, we learn today that infant diagnoses of GERD—gastroesophageal reflux disease—have skyrocketed in recent years. This is good news for the makers of Prilosec and other proton pump inhibitors, and as you might expect, the increased rate of diagnosis of infant GERD is largely because they’ve been aggressively marketing their pills for just this purpose. But guess what? It turns out that an awful lot of doctors are diagnosing GERD for any baby who’s spitting up and just generally crying a lot. However, for those babies—ones who don’t have objective evidence of GERD—randomized trials show that Prilosec and its cousins have no effect.
So what’s the answer? Well, how about if we tell parents that these drugs are ineffective? Amazingly enough, that doesn’t work. As the chart below shows, parent interest in the medication goes down only if you tell them it doesn’t work and you refrain from diagnosing GERD in the first place:
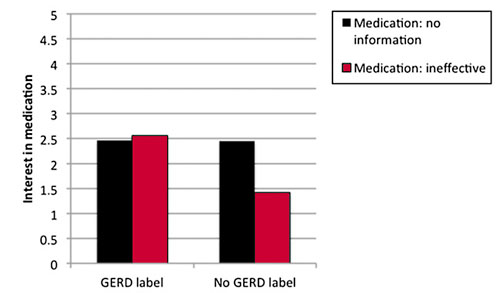
Gardner ruminates on the underlying cause of this: “Getting a diagnosis, I speculate, activated a mental schema that ‘my baby has reflux disease, therefore she needs an acid-reducing medicine,’ and this neutralized the information that ‘PPIs don’t work.’ So simply getting a diagnosis can have a harmful side effect on parents’ understanding of physician communication.”
So there you have it: once you put a label on an illness, people are more likely to want medication for it even if they’re explicitly told the medication doesn’t work. And this is even more important than it appears at first glance, since diagnoses of GERD vary from hospital to hospital by a factor of 13x. This may be a small example by itself, but those hospitals at the high end of the GERD curve are a perfect illustration of one of the reasons that healthcare in America costs so much.