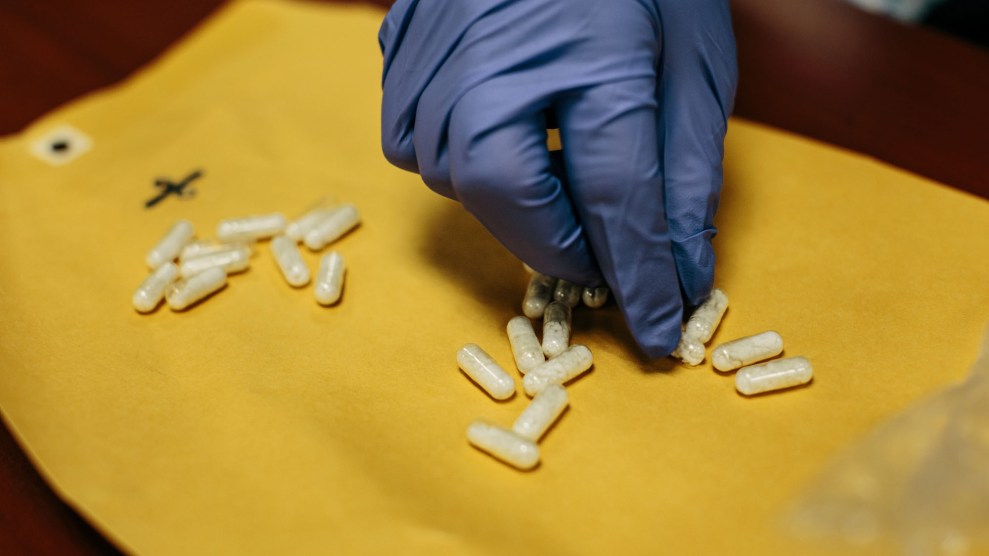
Stuart Ritchie/iStock/Getty
In the coming weeks, a federal task force will release highly anticipated recommendations on how to treat pain—and when to use opioids. It’s been a long time coming: As the opioid epidemic continues to claim lives, the medical community is struggling to lower prescription rates while making sure pain patients have access to medications they need. The Pain Management Best Practices Inter-Agency Task Force, a federal advisory committee operated out of the Department of Health and Human Services, was created to help prescribers strike the right balance.
There’s just one problem: Several of the task force’s 29 members have close ties to opioid makers. One doctor consulted for several opioid manufacturers in the early 2000s. Another received about $25,000 from OxyContin maker Purdue Pharma in 2017. Another member directs policy for the US Pain Foundation, which has received millions from opioid manufacturers. Until recently, committee chair Dr. Vanila Singh owned stock in Johnson and Johnson, a company facing charges in multiple lawsuits for its role in the opioid epidemic.
Drafts of the task force’s recommendations so far have taken a far more lax approach to opioid prescribing than previous federal guidelines on pain treatment. “It’s like going backwards,” said Dr. Anna Lembke, director of addiction medicine at Stanford University. The task force recommendations will not be binding, but federal guidelines tend to have a far-reaching impact, setting the tone for prescribers across the country. Opioid prescribing rates have slowly dropped off in recent years, but pharmaceutical companies, said Lembke, are eager for “any little opportunity for people to say, ‘No, it’s okay, you can prescribe.’”
Opioid makers lobbied to create a pain task force
The task force’s recommendations will not be the first attempt to guide opioid prescribing: In March 2016, the Centers for Disease Control and Prevention released historic guidelines urging doctors to limit prescriptions and, when possible, opt for non-opioid alternatives. Joint guidelines from Veterans Affairs and the Department of Defense followed the next year, taking an even firmer stance against prescribing opioids for chronic pain patients. Both publications presented a sharp contrast to the years-long industry-funded information campaign aimed at persuading doctors of the benefits of opioids.
Pharmaceutical companies took note of the changes. Three weeks before the CDC released its guidelines, Rep. Susan Brooks (R-IN), one of the House of Representatives’ top recipients of pharmaceutical funding, introduced legislation to create a task force that would review and update best practices on pain management and painkiller prescribing.
Opioid manufacturers and distributors lobbied heavily on the little-noticed bill, HR 4641. Endo, maker of Percocet, spent $1.8 million on the resolution and other opioid-related lobbying in 2016. Depomed, which makes opioid Nucynta, spent $170,000; the Healthcare Distribution Alliance, which represents several companies facing charges for their roles in the opioid epidemic, spent $1.2 million.
Ultimately, HR 4641 was wrapped into the Comprehensive Addiction and Recovery Act, the sweeping opioid legislation that passed in the summer of 2016, a few months after the CDC’s guidelines were released. The very first provision of the act stipulates that a range of stakeholders—including researchers, physicians, and patients representing both the chronic pain and addiction communities—“identify, review, and, as appropriate, determine whether there are gaps in or inconsistencies between best practices for pain management.”
An “undercover vehicle to influence federal policy”
Critics of the task force say it’s in thrall to an industry struggling to rebound from declining prescription rates. “Time and time again, opioid manufacturers have used tax exempt organizations they fund as an undercover vehicle to influence federal policy,” Sen. Ron Wyden (D-Ore.), who has spoken out about his concerns with the task force, told Mother Jones. “The latest example is the federal pain task force, which is being used as part of the industry’s broader effort to water down the CDC’s recommendations on opioid prescribing.”
Subtle yet significant differences distinguish the CDC’s guidelines from the task force’s draft, a final version of which will be released by the end of May. Perhaps the most contentious draft recommendation involves co-prescribing opioids and benzodiazepines, a class of tranquilizers including Xanax and Valium. Study after study has found the drug combination increases the risk of overdose, leading the CDC, the VA, and the Food and Drug Administration to warn against co-prescribing. The pain task force acknowledges the risks are “well established”—but recommends co-prescribing in some cases.
Lembke, the Stanford addiction director, worries that as is, the draft recommendations are “promoting the very same myths about opioid prescribing that got us into this mess in the first place: That no dose is too high, that risk assessment tools can predict who will get addicted, and that combining opioids and [benzodiazepines] has ‘clinical value.'”
A committee with conflicts of interest
At the first HHS task force meeting a year ago, four patients tearfully described the horrific reality of living with chronic pain. All of them took opioids and feared being forced off the drugs they relied on. “I take a really high amount, but I only take enough to where it keeps me able to function,” said one patient, a grandfather of three. Another patient explained that she had tried everything to cure her spinal pain, from physical therapy to regular injections, but opioids were also a part of her treatment tool box. “We’ve created a system where medications are often the most accessible, effective option, and yet we’re punishing patients for using that option,” she said. Their comments were echoed earlier this year, when the task force opened a public comment period and more than 5,000 responses flooded in. Many came from pain patients pleading for access to medications.
The problems the patients described—and much of the backlash to the CDC’s recommendations—stem from how the growing concerns about opioids’ addictive qualities have been codified into hard-and-fast policies. The CDC guidelines were intended as guidelines, not rules. But a number of insurance plans, pharmacies, and local and state governments have used them as justification for limiting the number of days patients can receive prescription opioids, leading to fears of forced tapers (which the guidelines explicitly warn against) and patient abandonment.
Given these challenges, the task force is supposed to represent the competing needs of two vulnerable populations: patients who rely on opioids for pain treatment, and patients who have suffered from the painkillers’ addictive effects. The 29-member task force, however, skews toward the former.
A number of members appear to have conflicts of interest with opioid makers, noted a letter from Sen. Wyden to Health Secretary Alex Azar last December. Dr. Rollin Gallagher consulted for Purdue Pharma, Endo, and opioid maker Janssen in the early 2000s. Today, Gallagher is the editor-in-chief of Pain Medicine, the flagship publication for the American Academy of Pain Medicine (AAPM), which received nearly $1.2 million from five largest opioid makers between 2012 and 2017, according to a Senate investigation. Dr. Jianguo Cheng, who recently finished his term as AAPM president, received a consulting fee of $24,600 in 2017 from Purdue—the eighth largest standalone payment Purdue made that year. Cindy Steinberg is the policy director for the US Pain Foundation, which received nearly $3 million in payments from the five biggest opioid makers from 2012 to 2017.
(Steinberg said that she doesn’t “know about or get involved in the finances” of the foundation, and that her advocacy is based on her personal experience with chronic pain. In a public letter, AAPM noted that industry funding supports conferences, ads, and educational and research grants—and should “never be interpreted as AAPM endorsing the products or services of these companies.” The letter also notes that Gallagher voluntarily gave up advisory relationships with medical companies more than ten years ago in order to ensure editorial independence, and that Cheng’s work with Purdue involved reviewing proposals to research non-opioid pain treatments.)
Task force chair Dr. Vanila Singh, a pain specialist at Stanford University, also has pharmaceutical ties: Last year, she spoke at conferences for AAPM and the American Academy of Integrative Pain Management, a recently shuttered organization that also received millions from opioid makers. Mother Jones found that Singh’s husband, a radiologist in California, received nearly $67,000 from former opioid maker Covidien in 2014. (Covidien sold a number of medical products; an HHS spokesperson declined to specify if the fee was opioid-related.) According to her 2017 financial disclosure form, Singh owned between $15,000 and $50,000 worth of stock in Johnson and Johnson, as well as stock in Philip Morris International.
It was an honor to speak as a panelist with @BobTwillman Academy of Integrative Pain Management #globalpaincliniciansummit2018 @cmoHHS #pain #opioids #nostigma pic.twitter.com/QA7WCx9uqc
— Vanila Singh,MD (@VanilaSingh) November 9, 2018
An HHS spokesperson said that Singh has since sold the stocks, and neither her participation in the conferences nor her husband’s association with Covidien created a conflict of interest. “We don’t agree that the committee is skewed in one direction,” the spokesperson said, adding that its members “represent an extremely diverse group of stakeholders and interests.” Since the task force is a federal advisory committee, some task force members are expected to expected to represent the interests of private stakeholders, the spokesperson said. “They are not government employees, so are not covered by the federal ethics laws.”
Assuming the task force releases recommendations similar to its current draft, physicians will soon face two conflicting federal guidelines: The CDC discourages opioid use and suggests baseline dosages if need be, while the pain task force encourages clinicians to rely on personal judgement. University of Southern California health policy professor Jason Doctor worries that the latter endorses an attitude that helped contribute to the epidemic to begin with. “We need to look to see what’s helpful and what’s harmful, and generally follow rules around that with some rare exceptions—not send clinicians out to make their own judgements,” he said. “Because that’s what we’ve been doing, and it hasn’t been working.”