Michael Rieger/Zuma
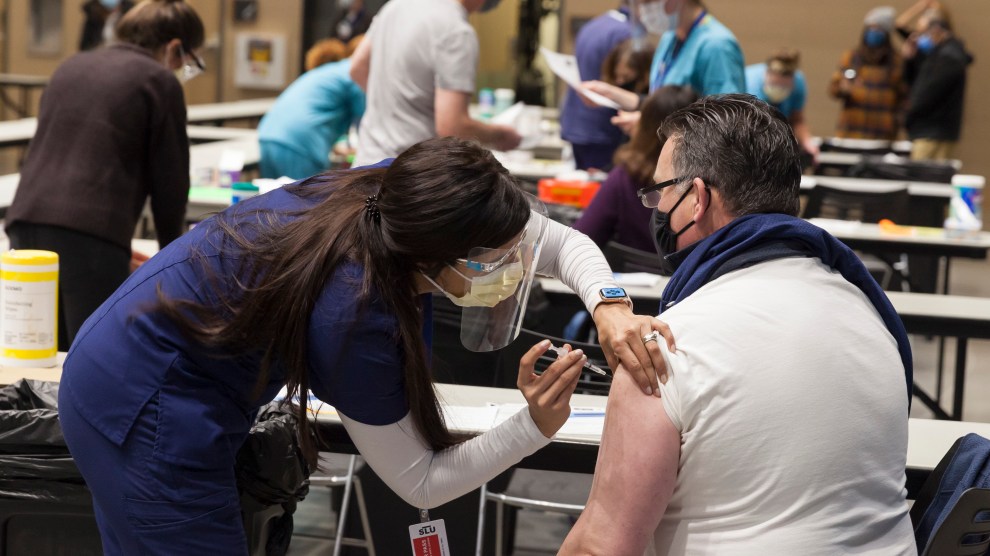
On Sunday, the Food and Drug Administration authorized a third coronavirus vaccine, produced by Johnson & Johnson, for emergency use. This one’s a little different: It’s more shelf-stable than the mRNA vaccines already in distribution, and requires just one dose. Sounds great, right?
Yet questions abound about the new vaccine—and the old ones, too. To clear up existing doubts about how these vaccines trigger an immune response and protect against the coronavirus, we consulted an expert—Dr. Jesse Goodman—who is the director of the Center on Medical Product Access, Safety and Stewardship at Georgetown University and a former chief scientist at the FDA.
Mother Jones: Public health experts, including Dr. Anthony Fauci, have said the best vaccine is whichever one you can get. Why is that?
Jesse Goodman: The needs and the demand for vaccine are far above what’s available. The virus is circulating at high levels, and vaccination is the best way people can protect themselves. All three vaccines that are currently available under emergency use in the US are very effective in preventing against severe disease, and that’s the main thing individuals need to worry about.
MJ: How does the technology of the Johnson and Johnson vaccine differ from that of the Pfizer or the Moderna vaccines?
JG: The Pfizer and Moderna vaccines use mRNA, which is the message the virus uses to make a protein. The vaccine mixes the RNA with little globules of fat, and when the mixture is injected into a cell, the cell produces the same spike protein that is normally present on the surface of the virus. The body’s immune system then makes antibodies and T cells that can kill the virus that has that same protein on its surface when it comes along.
Instead of using this naked RNA mixed in fat, the Johnson & Johnson vaccine uses DNA that carries the same genetic code for the spike protein inserted into the DNA of a kind of cold virus, an adenovirus, that has been engineered so it can’t replicate in a person. After vaccination, this adenovirus enters your cells, which use the DNA to make mRNA for the spike protein. The cell then uses that mRNA to produce the protein itself, and your body makes antibodies and T cells that, as with the mRNA vaccines, can then react to the spike protein and kill the virus when it tries to infect you.
RNA is very fragile, which is part of the reason that the Moderna and Pfizer vaccines require frozen storage and have limited shelf life once they’re thawed. Because the Johnson & Johnson vaccine doesn’t have that naked RNA, it’s much hardier. It can be frozen under normal conditions and then refrigerated for about three months. That provides advantages in transportation and handling in clinics and healthcare setting where freezing is not as practical. The other thing is that the Johnson & Johnson adenovirus vaccine produces a strong immune response after one dose.
MJ: Because the J&J vaccine is easier to ship and store, it’s likely to be deployed in harder-to-reach communities. How would you respond to the suggestion that this creates a two-tiered system in which marginalized people get the short end of the stick in terms of vaccine effectiveness?
JG: What we really want to do is prevent people from getting really sick, and getting hospitalized or dying, and the J&J vaccine appears to do a perfectly fine job with that. I’ve already been vaccinated, but if J&J had been available when I was vaccinated, I would have gladly taken it.
MJ: How does the Johnson & Johnson version stack up in terms of efficacy?
JG: The vaccines were not compared head to head; these were different studies done in different places at different times. But it does appear that in preventing all infections, the J&J vaccine in the one-dose regimen may not be as effective as the two-dose regimen of the RNA vaccine. In the part of the clinical study that took place in the United States, the J&J vaccine was about 72 percent effective in reducing overall infection, as opposed to 94 or 95 percent with the RNA vaccines. However, they all appear very highly effective in preventing severe manifestations that might require hospitalization or [cause] death.
MJ: Would taking two doses of the J&J vaccine boost its overall efficacy?
JG: We don’t know yet. J&J has a study going on now that looks at two doses. Still, there’s a tremendous advantage to getting vaccinated, if you can get any of these vaccines, because all three seem to really prevent the serious infections and complications that both make people sick and stress our health care system.
MJ: How effective are the mRNA vaccines if just one shot is administered?
JG: Information about that is limited, because virtually everyone in the clinical trials got a second shot. Between the first and second shot, depending on the vaccine and on how we look at the data, there was protection against infection on the order of somewhere from 50 to maybe 80 percent. So even after one dose, within a couple of weeks, there is some protection. What we don’t know is how long would that last without the second dose.
There is also some concern that incomplete immunity could worsen the problem by selecting for variant viruses. In other words, variant viruses might have an advantage over non-variant viruses in overcoming that low-level antibody that’s present after just one dose. It’s not proven, but it’s a reasonable concern.
MJ: How does the efficacy of a vaccine in a clinical trial relate to its effectiveness in the real world?
JG: Vaccines and drugs frequently look better in their clinical trials than they do when they’re out in the broader population because patients in clinical trials are often healthier. But so far, it looks like the very high levels of efficacy that were present in the clinical trials are being maintained as it’s brought out in the broader population. Part of the reason is that these trials were done with an emphasis on trying to incorporate people of all ages, including older people who often don’t respond as well to vaccines.
MJ: Does getting vaccinated lower the risk of having an asymptomatic infection and spreading the virus to others?
JG: We don’t have data yet on transmission. Our sense is that the vaccines will decrease transmission in the community and contribute to the health of both individuals and the public. Whether vaccines with higher efficacy will do a better job of that, we’ll hopefully know more in the future.
MJ: How long does immunity last?
JG: We don’t know. It could be that it differs among the vaccines, but right now there’s not a lot of strong information that there should be a strong preference for one or the other.
MJ: Are these vaccines safe and effective for pregnant women?
JG: Animal studies show no evidence of reproductive risk to mother or fetuses. There are no studies performed yet in pregnant women. However, a number of pregnant women have been vaccinated, and to date there is no evidence of adverse effects on the mother or fetus from the vaccines.
Pregnant women are at higher than average risk for getting bad outcomes from COVID-19 infection, and the CDC and the American College of Obstetricians and Gynecologists recommend that pregnant women get vaccinated if they otherwise meet eligibility criteria.
MJ: What about teenagers?
JG: Studies are underway, but there’s no data yet—with the exception of the Pfizer vaccine, which is authorized for people 16 and up.
MJ: When might we expect to see a vaccine approved for use in children?
JG: Those studies will probably not be available until late in the year.
MJ: Is there any fear that a variant could emerge that’s more dangerous for kids?
JG: The virus has kept throwing new things at us, and we still do not understand the multi-system inflammatory syndrome that COVID causes—fortunately, rarely—in children, so this question will need continuous monitoring.
MJ: How do these vaccines hold up against the more contagious variants of the virus?
JG: Some of the genetic variants somewhat lower the effectiveness of the vaccine. The J&J vaccine trials included people in South Africa and Brazil, where some of these variants seem to have originated. While effectiveness was reduced somewhat in those countries, maybe by about 10 percent, the good news is that the vaccines were still effective in preventing hospitalizations and deaths.
MJ: Suppose a vaccine-resistant variant were to emerge. Could we easily just tweak the existing vaccines?
JG: Studies are underway now at most of the major companies using vaccine variants to tweak the vaccines in case it’s needed. It wouldn’t be a completely new vaccine; it would be more like what we do for flu vaccines every year. If the virus changes, we make adjustments, and that can be done quite quickly, particularly for RNA vaccines.
MJ: How big of a threat is vaccine hesitancy to achieving herd immunity?
JG: That’s a real hurdle. There still are people who are concerned, and there needs to be an effective strategy of communication to those people if vaccines are really gonna have impact they can have. Being sure that people understand the ways in which vaccines may or may not be different, understand their benefits, understand their safety profile, those things are really important.
The pandemic seems to have these ups and downs that nobody fully understands. I worry that we could get to a place where events are not as dramatic as they were a month or two ago or back in the spring, and people could feel less urgency about getting vaccinated.
We really need to help people understand that there will be likely upticks again, there is the threat of these variants globally, and that being immunized is smart both to protect yourself, and your loved ones and your community.