yupiyan/Getty
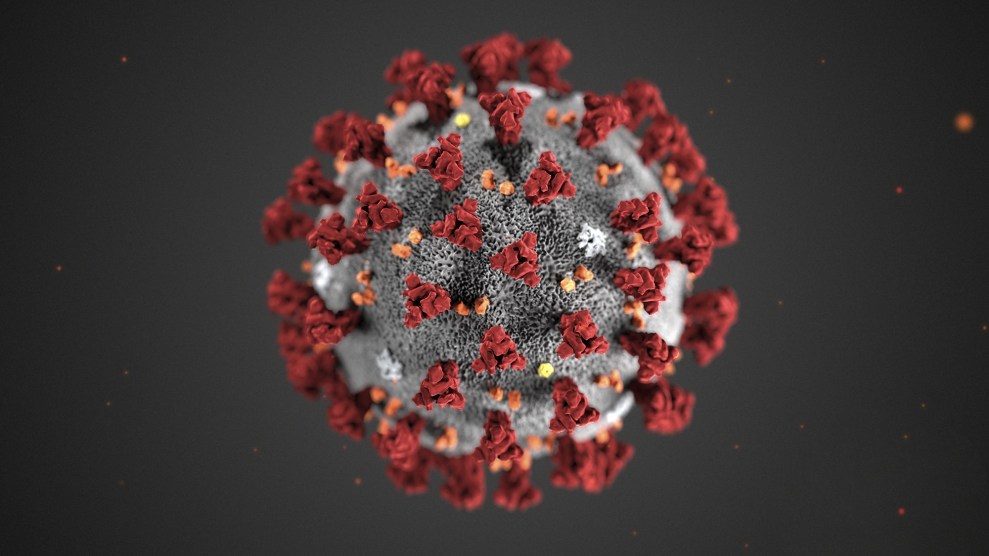
Last week, the Centers for Disease Control and Prevention warned that incidents of the coronavirus, which causes COVID-19, would increase in the United States and would likely disrupt daily lives. To contain the spread, health care experts advise constant hand-washing, avoiding close contact with anyone who is sick, and staying home if you suspect you have symptoms—which include fever and cough.
Of course, for the homeless population, those straightforward guidelines are close to impossible.
“Unfortunately, we know that people living in crowded, unsanitary conditions are at increased risk for a variety of infectious diseases,” Dr. Jeffrey Klausner, a public health and medicine professor at the University of California, Los Angeles, told the Los Angeles Times. The illness first appeared in China in December. According to the World Health Organization, more than 87,000 people have contracted the disease, and it has killed about 3,000 people worldwide—including six people in Washington state. Officials are urging calm. “While there is some spread in some communities there is no national spread of COVID-19 at this time,” Nancy Messonnier, director of the CDC’s National Center for Immunization and Respiratory Disease, said at a press conference on Saturday. But public health experts are worried about one population that could be especially vulnerable to the disease: people living in encampments or in community shelters.
“Housing is a public health issue,” says Dr. Tobie Smith, a public health professor at Georgetown University. The recommendations for staying safe from coronavirus are simple—if you have a stable place to live. For unsheltered people, there’s no home for self-quarantine, and they have only unpredictable access to public bathrooms for frequent hand-washing. Many unhoused people are already sick or have compromised immune systems, putting them at higher risk of death. Even for those in shelters, avoiding close contact is virtually impossible, as shelters aren’t built with quarantine rooms. For unhoused people, “the actual recommendations are just not feasible,” Dr. Smith says.
During the 2003 epidemic of SARS, a similar respiratory virus infected more than 8,000 people and killed 774 worldwide, but only eight people contracted the virus in the United States; they all had traveled to a country with infections. In Toronto, Canada, however, where there were 257 cases, there was growing concern that the homeless population was at risk. Advocates for unhoused people were not prepared to handle an outbreak: They could not figure out how to effectively communicate the danger to homeless individuals and families; they lacked supplies for proper disease screening; and they weren’t able to quarantine patients living in shelters. No homeless people were reported to have contracted SARS during the outbreak.
What are the options today for minimizing the risk to unhoused people? In Spokane, Washington, city officials are educating shelter workers on strategies for educating those who reside in homeless facilities on how to keep safe. Local nonprofits are training workers on how to spot people who may be infected. They’re following recommendations from the local health department, which include giving masks to anyone who may show symptoms, but not as preventative measures. (Coronavirus symptoms are similar to a common cold, so it can be difficult for homeless outreach workers to decide if an individual needs immediate attention.) In California, where there were 35 confirmed cases on Monday, the California Department of Health said it is monitoring the situation but has not yet released any specific plans.
An additional concern among public health officials is that an outbreak among homeless populations could lead to further stigmatization of an often marginalized group. Because homeless people lack access to health care and frequently move around and use public spaces like libraries and mass transit, the fear-mongering in the media has already begun—for example, an op-ed in a Seattle paper called for forcing homeless people into a shelter, lest they use public facilities and spread the illness. “This is not a reason to further marginalize these people,” Dr. Smith says, “but it shows how having people in our community who are unhoused is a threat in many ways.”