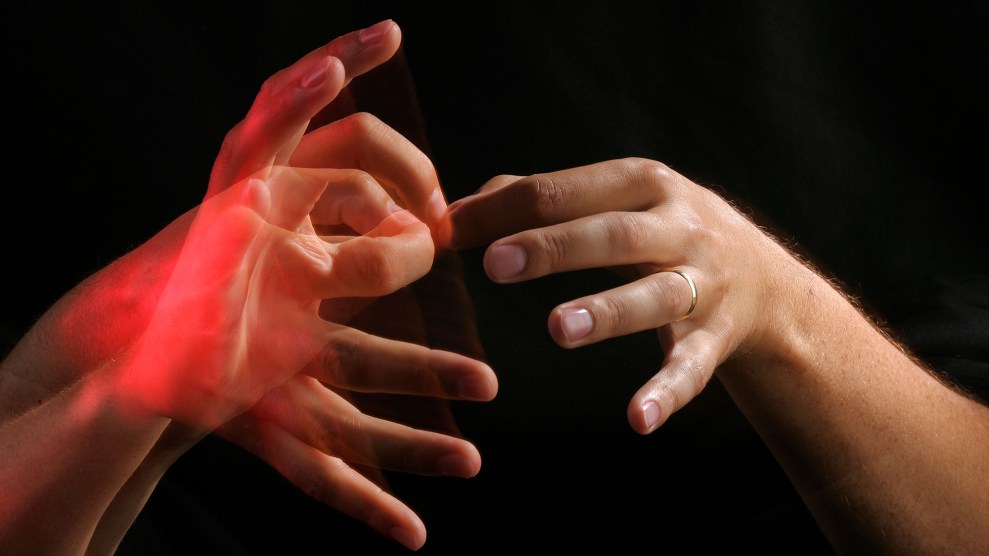
Mother Jones illustration; Getty
After more than five months of the coronavirus pandemic in the United States, White House briefings and press conferences still lack an American Sign Language interpreter. On Monday, a week after President Trump resumed his daily briefings, the National Association of the Deaf filed a lawsuit against the White House arguing that the continued refusal to include an interpreter violates the Americans With Disabilities Act. “All 50 states’ governors have provided in-frame American Sign Language (‘ASL’) interpretation during public briefings regarding the pandemic,” the lawsuit notes. “President Trump, however, does not. He now stands alone in holding televised briefings regarding the Covid-19 pandemic without ever having provided any ASL Interpretation.” The suit goes on to mention that other members of the White House coronavirus task force, including Dr. Anthony Fauci and Dr. Deborah Birx, also appear without interpreters.
For advocates in the deaf and hard-of-hearing communities, the White House press conferences have been a months-long reminder of unique challenges during the pandemic. Since the Americans With Disabilities Act was enacted 30 years ago, a number of measures have been taken to reduce discrimination against people with disabilities. In the years that followed, society-wide accommodations—like wheelchair ramps and closed captioning on television—were made to better integrate people with varying disabilities into the mainstream. But even with progress, the world isn’t particularly deaf-friendly, and COVID-19 has undercut many of the advances that have been made.
“The greatest challenges come from the lack of communication access that have been exacerbated by the pandemic,” Howard A. Rosenblum, the CEO of NAD, the group suing Trump, told me in an email last month. And those challenges range from high-level government communications to mundane interactions.
That was the case for Ashley, who’d lost much of her hearing when she was 15 months old and recently went to the Houston-area branch of America’s Best Contacts & Eyeglasses. The employees may have spoken louder so that she could understand them through their masks, but since she reads speech instead of signs, she asked them to lower their masks so she could understand what they were saying. They refused. After all, it was mid-July when cases of the coronavirus were spiking in Houston—on July 14, there were 2,962 new cases in the city on a single day.
Unable to read their expressions or understand what they were saying, Ashley (who asked that her last name not be used) became so frustrated and upset that she left the store—and left the state. She scheduled an appointment in her home state of Louisiana, a five-hour drive away, because even though masks are still required there, a mandate exempts those “trying to communicate with a person who is hearing-impaired.”
Like many others who are deaf or hard of hearing in the United States, Ashley relies heavily on speechreading to understand people. “My lifeline,” she calls it. Usually, Ashley would manage the demands of daily life, like trips to the grocery store or the optician, by letting “the person helping me know that I was hearing-impaired, I lipread so please be patient.” But that’s become complicated during the pandemic. As her experience at the Houston store illustrates, the new rules of engagement that create minor inconveniences for most people have become fundamental disruptions for many people who are deaf or hard of hearing.
“It’s already difficult being hearing-impaired in normal settings.” she says, “It’s a thousand times worse now that everyone is wearing a mask.”
Ashley’s interaction was troubling, but not unique. “People with hearing loss constantly say that it’s exhausting to communicate in these kinds of settings,” says Dr. Debara Tucci, director of the National Institute on Deafness and Other Communication Disorders at NIH, describing how social distancing and mask wearing have affected many people. “I think that this is going to go on for a very long time.”
A lot of people who can’t hear spend much of their lives making adjustments and compromises to fit a world of those who can. For deaf people, that means deploying a number of tools and strategies to communicate, such as manual language, technology, sometimes medical interventions like cochlear implants, and visual cues. But for the 48 million deaf or hard-of-hearing men, women, and children in the US, the massive social adjustments to combat the coronavirus have created a unique set of challenges—and not just for those who mostly rely on speech reading. American Sign Language, for instance, relies heavily on inferences from facial expressions. With voices muffled behind masks, the effectiveness of cochlear implants—ear implants that deliver sound by stimulating the auditory nerve—are reduced.
In mid-March, like millions of others, Robert Weinstock, interim director of public and media relations in the Office of University Communication at Gallaudet University, began working from home. Gallaudet University is in Washington, DC, and was chartered by Congress in 1864 to serve deaf university students. Today, courses are taught using English and American Sign Language. Weinstock, who lives in the tight-knit suburban Maryland community of Takoma Park, says neighbors regularly meet at council meetings to discuss local and national politics. Resources for deaf people existed on a provisional basis. When Weinstock and his wife, who is also deaf, wanted to attend those gatherings, an interpreter had to be arranged. When those gatherings moved online during the pandemic, an interpreter was not initially included. “We’ve contacted our mayor, who has arranged interpreters for the webinars,” he says. “She’s been very helpful, but my point is that we were not considered in the beginning of the planning stage.”
Like people who aren’t deaf, many deaf people have scrambled to shift as much conventional life online as possible. In March, Gallaudet sent students home and offered online classes and weekly seminars to keep students connected. In some ways the students were well-prepared. According to Weinstock, visual resources like videos and PowerPoint were already part of the Gallaudet curriculum, and all courses are typically taught in ASL, which can be used over Zoom. Since the shift to remote learning, 99 percent of Gallaudet students successfully finished the spring semester online, and ahead of the fall semester, students and faculty are taking online modules to learn techniques—like embedding ASL and closed captioning into video—for more seamless class instruction. Still, digital-only learning isn’t perfect, and the unexpected changes have created their own challenges.
“There are students all over the world,” he said. “Suppose class time is at 8 a.m. in DC. If they’re in California, that’s a 5 a.m. class. England that might be at noon, and that might affect somebody in India because they had to go home.”
For many who are deaf or hard of hearing, aspects of the pandemic that others take for granted have been challenging. As noted in the lawsuit against the White House, briefings from state and local officials on safety measures and virus prevalence may not have initially included ASL interpreters, but by April they were a feature of 47 governors’ emergency press conferences. By the time of the NAD lawsuit on Monday, it was all 50. When New York became the US epicenter of the coronavirus in March, Gov. Andrew Cuomo began giving daily briefings. Disability Rights New York, an advocacy group, filed a lawsuit citing a violation of the Americans With Disabilities Act and charging that the governor’s emergency television press conferences violated the ADA because they lacked a live interpreter. By April, Cuomo was sharing the screen with Arkady Belozovsky, a sign language interpreter.
Closed captioning may be one solution, but it has its own liabilities. “First, we need information at the same time that others are provided that information,” Weinstock says. “Second, yes, many of the televisions have captioning available, but caption quality is highly variable.”
The danger of being out of the loop during COVID-19 can become even greater when illness strikes and someone needs a hospital or health care facility. It’s often nearly impossible for someone who is deaf—with or without an acute illness—to navigate the complicated demands of accessing care. According to Tucci of the NIH, “There are so many issues in hospitals that are so busy, and understaffed, and under-resourced.” In health care facilities slammed by the pandemic, she says it’s possible that the essential question of accessibility for deaf patients wouldn’t “rise to the top.” The National Association of the Deaf established guidelines for hospitals and deaf patients in early April, and what NAD describes is troubling. “Many hospitals will not allow in-person interpreters, family members, or visitors to come into the hospital. You may be alone for a long time when you are in the hospital,” the website states. Guidelines recommend that patients bring a card stating, “PLEASE RESPECT MY LEGAL RIGHT TO UNDERSTAND YOU AND PARTICIPATE IN MY CARE BY ALLOWING ME TO USE THE SMARTPHONE,” to avoid medical decisions being made without legitimate consent from patients.
Beyond health care, experts in the field are also concerned about how heightened tensions between law enforcement and communities of color enter the equation when everyone is wearing masks. Recent deaths of unarmed people of color at the hands of police have shown the challenges disproportionately faced by members of more vulnerable communities as they navigate interactions with the police. Those encounters are especially difficult when someone can’t hear—or possibly speak. According to Vox, a quarter of those shot by police have a disability. With law enforcement wearing masks too, being able to interpret information clearly—and quickly—can be life-or-death. “I’ve had a number of conversations with mostly Black, Indigenous, and POC men who say they intentionally will wear a very cutesy mask in order to diminish any kinds of concerns,” says Teresa Blankmeyer Burke, a philosophy professor at Gallaudet. “If you are a deaf person and a police officer is shouting behind your back, you’re not going to know.” Even if they’re standing in front of you, that still may be the case.
As deaf and hard-of-hearing individuals adjust to the social code of the pandemic, the spaces where they might feel most at home—like schools or social organizations for deaf people—have also disappeared. Burke points out that for many deaf people who practice ASL, the most candid communication comes with other deaf people. She compares it to someone interacting in their home language with another native speaker. “I always have a little bit of a sigh of relief and relaxation when in a signing environment,” Burke says. “A lot of guess work goes into speech reading, so we cannot access language without using a lot more of our working memory or cognitive load. It’s much more mentally fatiguing for us, but in a signing community and using sign language, it’s less fatiguing.” With social distancing, those spaces are unavailable.
As the pandemic wears on, innovations have appeared, including third-party apps that add live closed captioning—which Zoom doesn’t offer itself. Voice-to-text phone apps transcribe dialogue in real time, and they’re becoming widespread even though there are problems with voice recognition software. Increasingly, masks are appearing that display the mouth through a sheet of clear plastic, but the plastic panel “tends to block the flow of sound,” Tucci says. It can also trap air and become uncomfortably hot. In hospitals and other medical facilities, certain provisions of HIPAA—a law designed to protect patient privacy—have been suspended during the emergency, so translators can be included in telehealth sessions, paving the way for clearer communication between providers and patients. “I’m the patient and trying to interact with the doctor, and I have this physical connection with this space and person, but the interpreter is in a box and they can’t see much,” says Erin Wilkinson, a deaf linguistics professor at the University of New Mexico. “That is really complex.”
Increased communication through screens and restricted physical interaction may have the potential to spark enduring linguistic changes for ASL users. After all, the migration of chat from analog to digital isn’t restricted to the world of health care. When deaf people rely on signing as their principle mode of communication, Wilkinson says, they generally “sign with people they know well.” But today, when so much communication is virtual, more deaf people are signing with more strangers, and the popularity of social media that’s video-focused—TikTok and Instagram, for instance—are more adaptable to ASL than other apps. “How do they modify their ASL to communicate with these people they’ve never met before?” Wilkinson asks. “That’s a very big question to research, because so far deaf people haven’t really had big experiences in communicating with people in ASL that they’ve never met before.” She also wonders about physical interactions between mask-wearing ASL users. If requirements to cover faces last long enough, what workarounds will appear in the absence of facial expressions to help decipher meaning?
Burke, the Gallaudet professor, sees an opportunity. She says that after the pandemic, the way deaf people interact with everyone could stop being an afterthought. Rather than deaf accessibility to Zoom in the form of an app update, it could be in the default product. She points out that the neighborhood around Gallaudet is like the border between two countries, where “people will pick up parts of the other’s language.” In non-hearing circles, Burke says, people are more patient in their communications and have to focus on each other. “In spoken-language communities, there is almost an affront when you miss something said,” she points out.
Fortunately for Ashley, that wasn’t the case during her eye exam in Louisiana. For much of the appointment, one of the assisting specialists pulled his mask down to speak. The entire exam took several minutes. It’s possible Ashley could have gotten her eyes checked closer to home. The ADA attempts to ensure that access to services in her life is no different than for anyone else. The demands of a five-hour drive across state lines are grueling, but when she arrived she knew that her needs and those of other deaf people were taken into consideration. Still, it was only one interaction of many. “This is a very frustrating time for everyone,” she says. “I like my independence, but now I feel like I need someone with me all the time.”